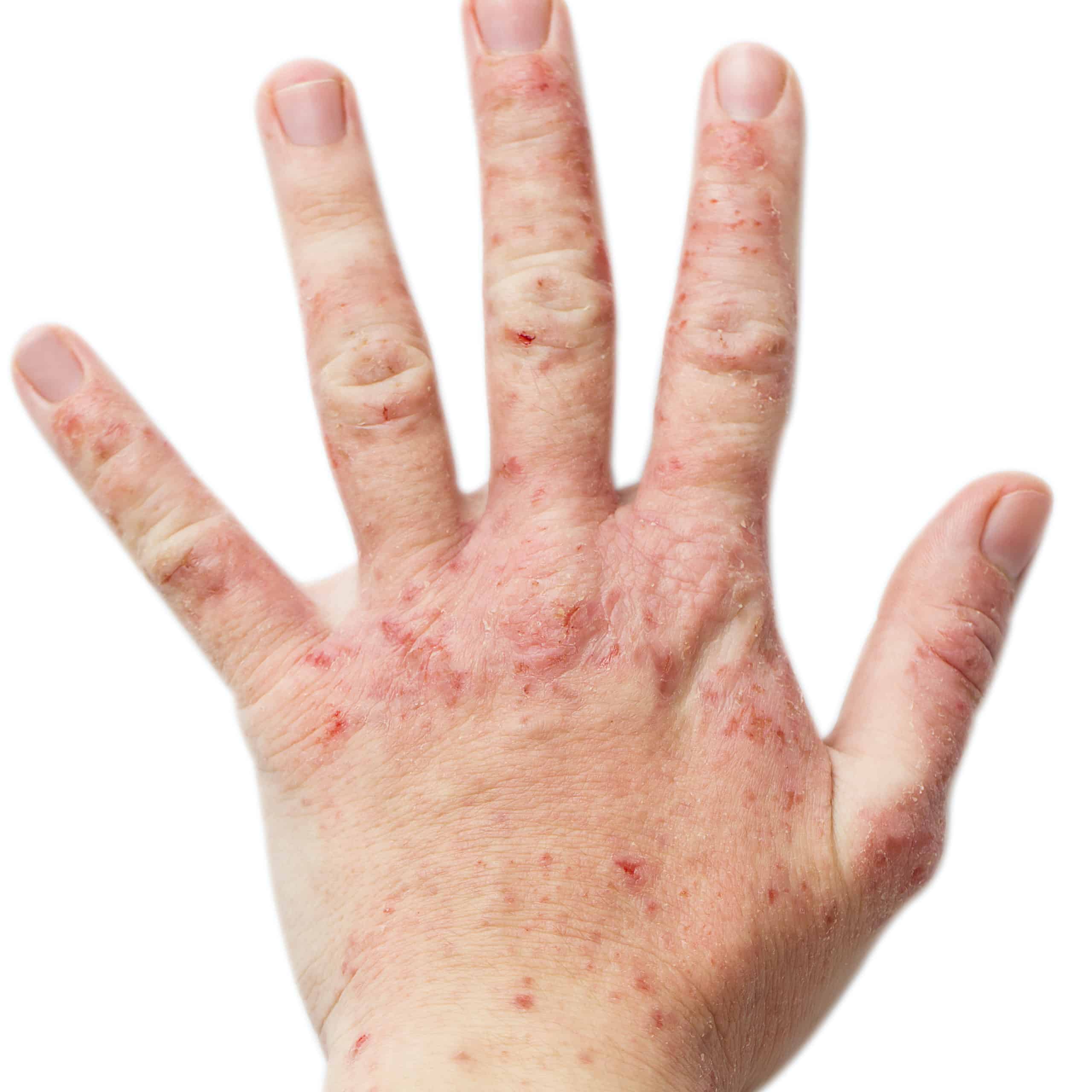
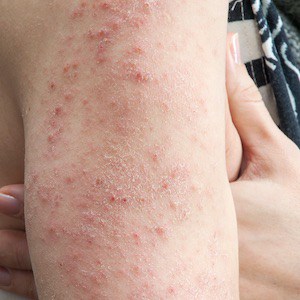
What is dermatitis?
The inflammation of the epidermis results in a number of changes in the appearance and texture of the skin.
The skin can become thicker, rougher, or hardened. It can also be excessively dry, resulting in cracking or flaking.
Dermatitis can be acute, meaning there is a sudden onset of symptoms. Or it can be chronic, needing long-term management.
Dermatitis can happen anywhere on the body. It’s often seen on the hands and neck, and the insides of the knee and elbow joints.
How is it caused?
As dermatitis covers a range of conditions, the causes vary from patient to patient.
For example, contact dermatitis is caused by irritation or allergic reaction to the things the skin comes into contact with. This can include a wide variety of substances, from water to wool and solvents to soaps.
Atopic dermatitis can be inherited genetically. It sometimes occurs in conjunction with hay fever and asthma.
Dermatitis can also be aggravated by stress and anxiety. It’s thought that higher levels of the hormone cortisol may affect the body’s usual immune systems.
Is dermatitis the same as eczema?
The names are sometimes used interchangeably as they both mean inflammation of the skin.
Often when doctors refer simple to “eczema” they mean atopic dermatitis. If the inflammation has been caused by physical contact, it will usually be referred to as irritant contact dermatitis or allergic contact dermatitis.
Why is it treated?
The inflamed skin can be red and rough. Particularly when this is on visible areas such as the neck and hands, patients are keen to return the skin to its usual appearance.
When the inflamed skin is thick and dry, it will crack and split easily. This can be painful when the skin is flexed, and can also pose an infection risk.
Diagnosis
A Dermatologist (specialist skin doctor) will examine the skin and take a full history. They’ll be looking to learn about any triggers or patterns in your symptoms. They’ll also be learning about any previous treatment you’ve tried at home or been prescribed by your GP.
There are a number of skin conditions that have similar symptoms. So the Dermatologist will be asking questions that help them to identify the specific condition you have, so that they can recommend the most suitable course of treatment.
Treatment
The best approach to treatment depends on the patient’s combination of triggers and symptoms.
General guidance recommended might include:
- Changes to washing routines, and reduced contact time with water.
- Reduced contact time with identified irritants.
- Depending on the patient, this may include specific fabrics, chemicals, soaps, detergents and dust.
Prescribed medical interventions may include:
- Topical steroid cream or ointment.
- Soap substitute cleanser with moisturising and antibacterial components.
- Specific moisturisers (emollients). Trial and improvement may be necessary.
- Antihistamines to reduce irritation.
- Oral or injected steroids in specific acute cases.
Once an effective combination of treatments has been found, symptoms usually improve within a matter of weeks.
Ongoing management is important as dermatitis often reoccurs. Treatment should be resumed when the patient becomes aware of returning symptoms. If this does not resolve the symptoms to the same degree, further changes can be made to the prescribed treatment.